General Topics
What Is A Pediatric Dentist?
A pediatric dentist has an extra two to three years of specialized training after dental school and is dedicated to the oral health of children from infancy through their teenage years. Children, pre-teens, and teenagers all need different approaches to deal with their behavior, guide their dental growth and development, and help them avoid future dental problems. A pediatric dentist is best qualified to meet children’s needs of all ages.
Why Are The Primary Teeth Important?
It is very important to maintain primary teeth health. Neglected cavities frequently lead to problems that affect developing permanent teeth. Primary teeth – or baby teeth – are important for (1) proper chewing and eating, (2) providing space for permanent teeth and guiding them into the correct position, and (3) permitting normal development of jaw bones and muscles. Primary teeth also affect the development of speech and add to an attractive appearance. While the front 4 teeth last until 6-7 years of age, the back cuspids and molars aren?t replaced with permanent teeth until age 10-13.
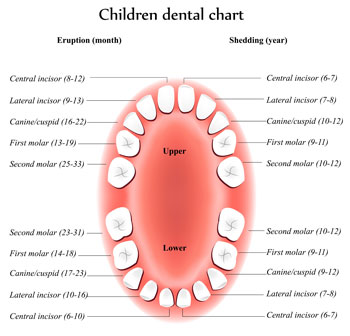
Eruption Of Your Child's Teeth
Permanent teeth begin appearing around age 6, starting with the first molars and lower central incisors. At age 8, you can generally expect the bottom 4 primary teeth (the lower central and lateral incisors) and the top 4 primary teeth (the upper central and lateral incisors) to be gone and permanent teeth to have taken their place. There is a one to two-year break from ages 8-10, and then the rest of the permanent teeth will start to come in. This process continues until approximately age 21.
Adults have 28 permanent teeth or up to 32 including the third molars (called wisdom teeth).
Dental Emergencies
Cut Tongue, Lip, or Cheek: Apply ice to the affected area(s). If there is bleeding, apply firm but gentle pressure with a gauze or cloth. If the bleeding cannot be controlled by simple pressure, call a doctor, or visit the emergency room.

Knocked-Out Permanent Tooth: If possible, find the tooth. Handle the tooth by the crown, and be careful not to touch the root portion. You may rinse the tooth but DO NOT clean or handle the tooth excessively. Inspect the tooth for fractures. If it is sound, try to reinsert it in its socket. Hold the tooth in place by gently biting on a gauze or clean cloth. If you cannot reinsert the tooth, place the tooth in a cup containing the saliva of the person that lost it or use milk, but NOT water. The tooth may also be carried in the mouth beside the cheek. The person who lost their tooth must see a dentist IMMEDIATELY! Time is a critical factor in saving the tooth.
Knocked Out Baby Tooth: Contact your pediatric dentist. Unlike a permanent tooth, the baby tooth should not be replanted due to possible damage to the developing permanent tooth. In most cases, no treatment is necessary.
Chipped/Fractured Permanent Tooth: Time is a critical factor, contact your pediatric dentist immediately to reduce the chance of infection or the need for extensive dental treatment. Rinse the mouth with water and apply a cold compress to reduce swelling. If you can find the broken tooth piece, bring it with you to the dentist in a glass of milk, or the person’s saliva. DO NOT USE WATER TO TRANSPORT A CHIPPED TOOTH.
Chipped/Fractured Baby Tooth: Contact your pediatric dentist.
Severe Blow to the Head: Call 911 immediately or take your child to the nearest emergency room.
Possible Broken or Fractured Jaw: Keep the jaw from moving and take your child to the nearest emergency room.
Read more about how to prevent dental emergencies during recreational activities and sports with mouth guards.
Dental Radiographs (X-Rays)
Radiographs allow dentists to diagnose and treat health conditions that cannot be detected during a clinical examination, and they detect much more than cavities. For example, radiographs may be needed to survey erupting teeth, diagnose bone diseases, evaluate the results of an injury, or plan orthodontic treatment. If dental problems are found and treated early, dental care is more comfortable for your child and more affordable for you.
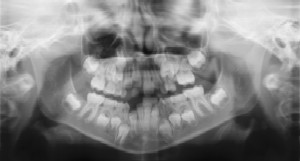
The American Academy of Pediatric Dentistry recommends radiographs and examinations every six months for children with a high risk of tooth decay. On average, most pediatric dentists request radiographs approximately once a year. Approximately every 3 years, it is a good idea to obtain a complete set of radiographs, either a panoramic and bitewings or periapicals and bitewings.
Pediatric dentists are particularly careful to minimize the exposure of their patients to radiation. With contemporary safeguards, the amount of radiation received in a dental X-ray examination is extremely small. The risk is negligible. In fact, dental radiographs represent a far smaller risk than an undetected and untreated dental problem. Today’s equipment filters out unnecessary x-rays and restricts the x-ray beam to the area of interest. High-speed film and proper shielding assure that your child receives a minimal amount of radiation exposure.
What's The Best Toothpaste For My Child?
Use only a smear of toothpaste (the size of a grain of rice) to brush the teeth of a child less than 3 years of age. For children 3 to 6 years old, use a pea-sized amount of toothpaste and perform or assist your child’s toothbrushing. Remember that young children do not have the ability to brush their teeth effectively on their own. Children should not swallow excess toothpaste after brushing

Does Your Child Grind His Teeth At Night? (Bruxism)
Parents are often concerned about their children grinding their teeth while they sleep (bruxism). Often, the first indication of bruxism is the noise created by the grinding, or, the parent may notice teeth wearing down. One theory is that psychology affects bruxism. Stress due to a new environment, divorce, changes at school, etc. can influence a child to grind their teeth. Another theory links pressure in the inner ear. If there are pressure changes (like in an airplane during take-off and landing, when people are chewing gum, etc.) the child will grind by moving their jaw to relieve this pressure.
The majority of cases of pediatric bruxism do not require any treatment. If excessive wear of the teeth – attrition – is present, then a nightly mouth guard may be prescribed. The good news is that most children outgrow bruxism. The grinding typically decreases between the ages of 6-9 and children tend to stop grinding altogether between ages 9-12. If you suspect bruxism, discuss this with your pediatrician or pediatric dentist.
Thumb Sucking
Sucking is a natural reflex in infants and young children. They may use thumbs, fingers, pacifiers, and other objects on which to suck. It makes them feel secure and happy or provides a sense of security during difficult periods. Since thumb sucking is relaxing, it may induce sleep.
Thumb sucking that persists beyond the eruption of the permanent teeth can cause problems with the proper growth of the mouth and tooth alignment, and the intensity at which a child sucks on fingers or thumbs will determine whether or not dental problems may result. Children who rest their thumbs passively in their mouths are less likely to have difficulty than those who vigorously suck their thumbs.
Children should cease thumb sucking by the time their permanent front teeth are ready to erupt. Usually, children stop between the ages of 2 and 4. Peer pressure causes many school-aged children to stop.
Pacifiers are no substitute for thumb sucking. They can affect the teeth essentially the same way as sucking thumbs. However, pacifier use can be controlled and modified more easily than the thumb or finger habit. Consult your pediatric dentist if you have concerns about thumb sucking or pacifier use.
A few suggestions to help your child quit thumb sucking:
- Children often suck their thumbs when feeling insecure. Focus on correcting the cause of anxiety, instead of the thumb sucking.
- Children who are sucking for comfort will feel less inclined to indulge the habit when their parents provide comfort.
- Reward children when they refrain from sucking during difficult periods, such as when being separated from their parents.
- Your pediatric dentist can encourage your child to stop sucking and explain what could happen if they continue.
- If these approaches don’t work, remind your child of their habit by bandaging the thumb or putting a sock on their hand at night. Your pediatric dentist may recommend the use of a mouth appliance.
What Is Pulp Therapy?
Inside the tooth, under the enamel and a hard layer called the dentin, is a soft tissue called pulp. The pulp contains blood vessels, nerves, and connective tissue and creates the hard tissues surrounding the tooth during development. The pulp extends from the crown of the tooth to the tip of the roots – where it connects to the tissues surrounding the root. The pulp is important during a tooth’s growth and development The purpose of pulp therapy in Pediatric Dentistry is to maintain the vitality of the affected tooth so that the tooth is not lost.
Dental caries (cavities) and traumatic injury are the main reasons for a tooth to require pulp therapy. Pulp therapy is often referred to as a “nerve treatment”, “children’s root canal”, “pulpectomy” or “pulpotomy”. The two common forms of pulp therapy in children’s teeth are the pulpotomy and pulpectomy.
A pulpotomy removes the diseased pulp tissue within the crown portion of the tooth. Next, an agent is placed to prevent bacterial growth and to calm the remaining nerve tissue. This is followed by a final restoration, which is usually a stainless steel crown.
A pulpectomy is required when the entire pulp is affected by the root canal of the tooth. During this treatment, the diseased pulp tissue is completely removed from both the crown and root. The canals are cleansed, disinfected and, in the case of primary teeth, filled with a resorbable material. Then, a final restoration is placed. A pulpectomy for a permanent tooth would be filled with a non-resorbing material.
What Is The Best Time For Orthodontic Treatment?
Stage I – Early Treatment: This period of treatment encompasses ages 2 to 6. At this young age, we are concerned with underdeveloped dental arches, the premature loss of primary teeth, and harmful habits such as finger or thumb sucking. Treatment initiated during this stage of development is often very successful and many times, though not always, can eliminate the need for future orthodontic/orthopedic treatment.

Stage II – Mixed Dentition: This period covers the ages of 6 to 12, with the eruption of the permanent incisor (front) teeth and 6-year molars. Treatment concerns deal with jaw mal-relationships and dental realignment problems. This is an excellent stage to start treatment when indicated, as your child?s hard and soft tissues are usually very responsive to orthodontic or orthopedic forces.
Stage III – Adolescent Dentition: This stage deals with the permanent teeth and the development of the final bite relationship.
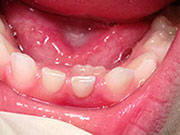
Adult Teeth Coming in Behind Baby Teeth